Eczema and psoriasis are often interchanged. Both skin diseases have visible red marks and rashes that may also come with a burning sensation, itchiness, and discomfort.
However, the two vary when it comes to their causes and treatment of symptoms.
In this article, we’ll talk about the difference between eczema and psoriasis and how they identify with one another.
Table of Contents
Eczema and psoriasis: A quick overview
The two conditions are common skin diseases that show signs of red spots that often lead to pain and discomfort. In the eyes of laypeople, these marks may all seem the same. But these diseases are more than what it shows from the surface.
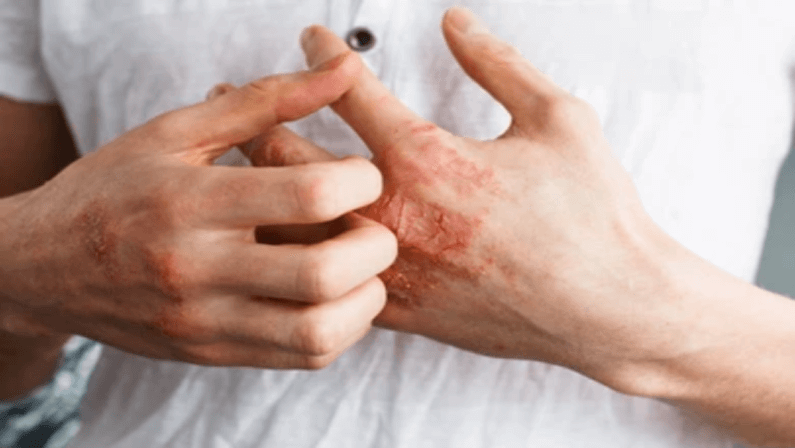
What is eczema?
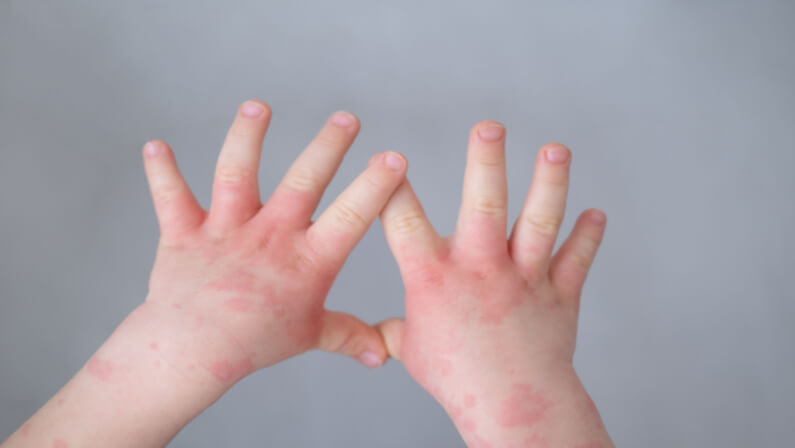
Eczema, also known as atopic dermatitis, is a skin condition that leads to dryness and inflammation. The disorder typically develops among children and can be a long-term condition.
The symptoms of people with eczema vary from person to person. But there are common signs that include itchiness, cracked skin, raised bumps, and crusting of the affected surface. The common triggers of eczema are allergy and infection.
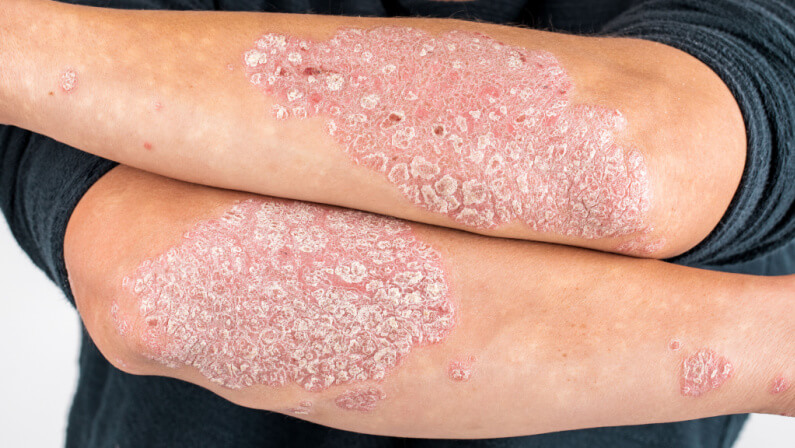
What is psoriasis?
Psoriasis is a condition that results in scaly patches that mostly appear on the knees, elbows, and trunk. The pain from psoriasis often interferes with sleep. It also makes you lose focus.
This chronic disease has no cure. It often flares up for weeks or months before subsiding for a while. Triggers for psoriasis include infection, burns, and medications.
Eczema and psoriasis are entirely different diseases. That is why you need to consult a dermatologist to know your exact condition before getting any treatment.
A skin specialist knows what’s the difference between psoriasis and eczema upon initial check-up.
Book an appointment with Team Dermatology in its Houston and Sugar Land locations if you have symptoms of any of the two and to assess what type of skin disorder you may have.
What do eczema and psoriasis have in common?
Eczema and psoriasis are both common skin diseases that affect millions in the United States. There are over 7.55 million with psoriasis, while there are 31.6 million who deal with eczema.
Below are the similarities of both diseases.
- The appearance of the skin. Both disorders present cracked and scaly skin that is often dry, sensitive and has a burning sensation when touched.
- Non-infectious. Psoriasis and eczema are not contagious. The diseases cannot pass from one person to another.
- Genetically-inherited. The conditions may be hereditary
- No cure. Eczema and psoriasis are both chronic conditions that have no cure. However, there are treatments to reduce their symptoms and ease discomfort.
- Affects anyone. Psoriasis and eczema can affect people of any age, gender, and race.
Differences between eczema and psoriasis
While there may be similarities between the two disorders, their difference is far broader.
Below are the details if you are wondering what’s the difference between eczema and psoriasis in adults.
When they first occur
Psoriasis starts during early adulthood and lasts later in life. Eczema also develops at any time. However, it is most common among children. An allergic reaction usually triggers the condition.
Appearance
For plaque psoriasis, the skin is red with silver scales. They are mostly raised and painful when touched. The plaques are thicker and drier than eczema.
Location
Psoriasis appears mainly in the face, scalp, fingernails, lower back, knees, palms, and feet. On the other hand, eczema in adults develops around the eyes, neck, hands, feet, and ankles.
Fluid
Eczema forms fluid within its patches that leaks through the skin. This condition is named serious exudate or weeping eczema. The fluid comes from the skin’s inflammation and may cause severe skin infections.
Psoriasis, meanwhile, does not develop fluid as they are drier.
If you have eczema and notice fluid that comes out of your patches, book a consultation immediately with Team Dermatology to address the issue with a dermatologist.
Triggers
Is psoriasis different than eczema when it comes to triggers? Yes, the causes of the diseases also vary.
The most common triggers of atopic dermatitis are changing weather, stress, exposure to tobacco, and allergens.
On the other hand, psoriasis flare-ups can be from cuts and abrasions, cold and dry weather, and infections like strep throat. Harsh soaps and skin products also cause psoriasis to flare up.
Itchiness
Eczema can cause more itchiness in the skin than psoriasis. During warm and hot weather, sweating from people with eczema may cause intensive itchiness. Meanwhile, psoriasis leads to discomfort during dry weather.
Can eczema become psoriasis?
Eczema and psoriasis are two diverse conditions. The diseases only develop from mild to severe, but they never become another form of the condition. Thus, eczema cannot turn into psoriasis.
Treatment options for both eczema and psoriasis
Treatment for eczema and psoriasis varies depending on the severity of the condition. Mild symptoms of the conditions can be addressed with home remedies, topical treatments, and lifestyle changes.
For moderate to severe conditions, you may need to consult a doctor for a different treatment level involving therapy and medications.
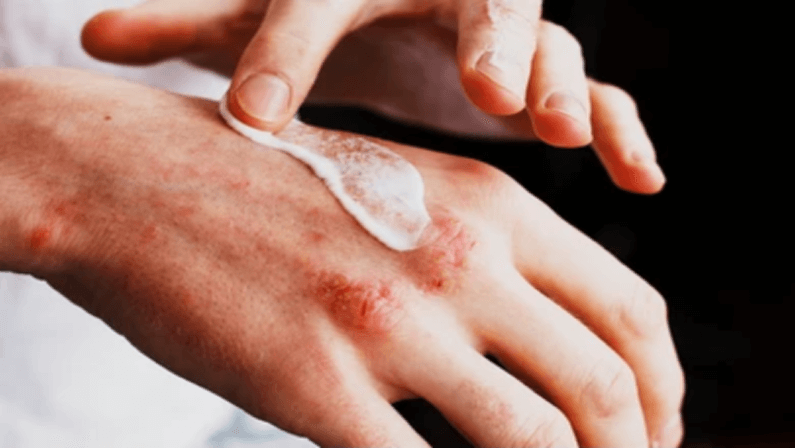
Try safe at-home remedies
Using moisturizers, mild soaps, and body cleansers help in reducing common symptoms of both diseases. Rashes and inflammation can ease if you use natural products such as colloidal oatmeal baths, apple cider vinegar mixed with water, and coconut oil.
Keep your skin hydrated
You can limit the symptoms of eczema and psoriasis with proper skin hydration. Moisturizing the skin helps manage dryness so it will not lead to itchiness and potential infection.
Take care of yourself
Developing proper health habits goes a long way to keeping your symptoms of eczema and psoriasis at bay.
Quit smoking and drink alcohol in moderation. You also need to have regular exercise and keep yourself hydrated—all these help keep your skin healthy.
Follow a healthy diet
Your dermatologist may advise you to switch to a Mediterranean diet proven to be heart-friendly. This diet boosts your body with nutrients that release anti-inflammatory properties.
Over-the-counter relief
Allergies are the most common trigger of eczema. Your doctor may recommend you take antihistamines such as diphenhydramine and cetirizine to curb inflammation.
Many OTC treatments help reduce inflammation and redness. Whether the medications are branded or in generic forms, these OTC reliefs also have sedatives that can aid in keeping you comfortable at sleep. You may have OTC pain relievers for symptoms of burning pain on the skin’s surface.
Meanwhile, your psoriasis symptoms may go down with retinoid, which you can get over-the-counter.
Retinoids reduce skin cell production, which may lessen flare-ups and inflammation. However, retinoids are not advised if you are pregnant or plan to get pregnant.
Topicals
A standard topical treatment that is effective for eczema is hydrocortisone. It comes in ointments, gels, and creams, which reduce skin irritation and relieve itching.
An OTC hydrocortisone can be applied up to four times daily for seven days.
Meanwhile, corticosteroids are given for mild to moderate psoriasis. Aside from ointments and creams, they also come in sprays and shampoos, which can be used if you have red scales on your scalp.
Topicals are for widespread patches in sensitive areas such as the face and skin folds. Use corticosteroids once a day during flare-ups or on alternate days.
Your healthcare provider may recommend a more substantial variety of this topical treatment for areas that are tough to treat. You only use the cream during flare-ups as long-term use of this may thin your skin.
Phototherapy
Phototherapy, or light therapy, is the first-line treatment if you already have moderate to severe psoriasis. It is a treatment that involves exposing the areas of your skin to controlled light or natural light repeatedly.
Your physician may recommend you to have phototherapy along with medications, depending on your case’s severity.
Light therapy also relieves inflammation and itching for eczema in adults and children. It is recommended after topical treatments prove to be inadequate.
However, its effectiveness is only for a while. You may need to undergo light therapy again if symptoms begin to re-occur.
Biologics
Biologics are drugs administered through injection. They suppress the immune system and interrupt the development of the disease’s signs and symptoms within weeks.
For psoriasis patients, biologics include apremilast (Otezla) and etanercept (Enbrel), among others. These decrease flare-ups and severe inflammation.
Biologics for eczema are dupilumab and tralokinumab, categorized as monoclonal antibodies that block the inflammation process. They also strengthen the immune system from germs that may infect sensitive skin.
Systemics
Systemics are a treatment for extreme psoriasis and eczema cases where topical medications are inadequate.
If you have psoriasis left untreated by topical medications and phytotherapy, systemic drugs are your choice. Most physicians prescribe acitretin, a type of retinoid that affects the growth of skin cells.
With severe atopic dermatitis, systemic corticosteroids such as prednisone and prednisolone are injected into the muscles to treat flare-ups.
Systemic treatments may cause serious side effects for both conditions. Your physician will have to monitor your treatments thoroughly to avoid serious consequences. If you are pregnant or planning to conceive in the next three years, systemic drugs are not for you as these medications can result in congenital disabilities.
Talk to a skin specialist for eczema and psoriasis treatment
Whether you have eczema or psoriasis, you need to visit a skin specialist to know the proper treatment. While home remedies may be effective for mild cases, you have to seek an expert to prevent your symptoms from flaring up, which may become a severe condition once left untreated.
Team Dermatology offers various treatments for skin diseases such as eczema and psoriasis.
Our skin experts specialize in dermatology and have a proven track record of treating mild to severe symptoms of both disorders. Book a consultation with us today to start your treatment.